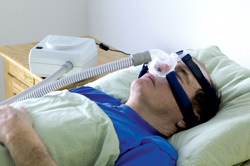
Rheumatoid arthritis hurts the whole body
Taking care of a patient with rheumatoid arthritis involved a partnership between internists and subspecialists, agree physicians managing cardiovascular risks, cancer or infections.
When internists think about chronic diseases that are associated with cardiovascular disease, rheumatoid arthritis (RA) isn't usually at the top of the list.
“Nobody questions when a diabetic comes to your office: Do we need to be thinking about cardiovascular comorbidity? Do we need to be managing this? When a rheumatoid [patient] comes to your office, you should be thinking the same thing,” said Beth L. Jonas, MD, assistant professor of medicine and director of the rheumatology fellowship training program at University of North Carolina-Chapel Hill.
According to recent studies, patients who have rheumatoid arthritis may face cardiovascular risks at least as elevated, if not higher, than those of diabetics, Dr. Jonas explained during a session at Internal Medicine 2010, held in April in Toronto.
She and other rheumatology experts interviewed on the topic would also like to draw internists' attention to other risks associated with RA, including cancer and infection. Whether the problems are caused by the disease itself or side effects from the medications that treat it, both specialists and generalists should be on the lookout, the experts advised.
“Taking care of a patient with rheumatoid arthritis should be a partnership between internists and rheumatologists,” said James R. O’Dell, FACP, a professor of medicine in the rheumatology section at the University of Nebraska.
Cardiovascular risks
The wider risks of RA may be more likely to come to mind if one remembers that it's not just a disease of the joints.
“Rheumatoid arthritis is a systemic disease,” said Dr. O’Dell. “Patients have premature mortality largely because of an excess incidence of coronary artery disease, to a lesser extent strokes, and it has everything to do with the inflammation that rheumatoid arthritis causes.”
In fact, studies have shown that even before patients develop clinical RA, they can have inflammation to an extent that it negatively affects their arteries. Making the highest-risk patients even harder to spot, research has indicated that traditional cardiovascular risk factors are not as predictive in RA patients.
Male sex, smoking and personal cardiac history have a lower impact on cardiovascular disease in RA patients than the general population, Dr. Jonas said. And in RA patients, low body mass index is actually a predictor of cardiovascular disease. “Oftentimes, the patients at highest risk are the skinniest ones,” she said.
Cholesterol in RA is also tricky, with some patients having low cholesterol or low triglycerides in the months to years preceding disease onset, said Dr. Jonas.
“In rheumatoid arthritis, there appears to be the development of a kind of HDL that is not as effective as the normal [kind],” noted Daniel E. Furst, FACP, professor of rheumatology at the University of California, Los Angeles.
Rheumatologists are debating how to treat cholesterol in RA patients. An ongoing statin trial won't have information published for another two to three years, according to Daniel Solomon, MD, MPH, associate professor of medicine at Harvard Medical School and chief of the section of clinical sciences in rheumatology.
In the meantime, some rheumatologists think the benefits of statins are enough that physicians should use them aggressively. “They have anti-inflammatory effects and those anti-inflammatory effects actually are helpful against the rheumatoid arthritis itself, so we have a very low threshold for getting people on statins if they have rheumatoid arthritis and a little bit of elevation of their LDL,” said Dr. O’Dell.
The relationship between reducing arthritis inflammation and cardiac risk also remains somewhat uncertain. It seems that RA treatments that reduce inflammation in the joints should do the same for the cardiovascular system, but it's not entirely proven.
“There are a number of studies that have shown that tight control [of arthritis] improves your cardiovascular risk. But I would say there are probably as many papers that say there's not any change,” said Dr. Jonas.
Dr. Furst thinks there is a double benefit, however.
“Any drug which is truly effective in decreasing inflammation in the patient—i.e., establishing remission—will ultimately decrease the risk of ASCVD [atherosclerotic cardiovascular disease],” he said. Specifically, hydroxychloroquine and chloroquine can decrease hyperlipidemia, and drugs that inhibit tumor necrosis factor-alpha (TNF) may reduce risk despite increasing cholesterol, he said.
In contrast, corticosteroids, which were a traditional treatment for RA, may increase risk.
“I would suggest limiting steroids, although some people think steroids may be somewhat helpful. I really think that the risks outweigh the benefits,” said Dr. Jonas. Internists should also be cautious about non-steroidal anti-inflammatories in these patients because of the possible association with cardiovascular problems, she advised.
Aspirin, on the other hand, should be used, perhaps to the same degree that it is in diabetics, Dr. Jonas said. “I don't put all my rheumatoids on aspirin de novo, but if you have patients who are at high risk, who have long-standing disease, who have other comorbidities, then I would put them on low-dose aspirin.”
Cancer risks
If the effect of drug treatment on rheumatoid patients' risk of cardiovascular disease seems complicated, the situation only gets more so in the case of cancer risks.
The evidence is clear that rheumatoid arthritis is associated with increased risks of certain cancers. “People with rheumatoid arthritis have about a two-fold increased risk of developing lymphomas and have a greater than normal risk of developing lung cancers,” said Dr. O’Dell.
Lung cancer risk may be an effect of the habits of the patients. Smokers have a significantly increased risk of developing rheumatoid arthritis. When they develop rheumatoid arthritis, it's more often severe and unresponsive to therapy, said Dr. O’Dell. (That can be a useful argument for convincing your RA patients to quit smoking, he noted.)
The cause of the lymphomas is less certain. “There is an inherent risk of lymphomas in rheumatoid arthritis, independent of treatment. There is controversy regarding whether TNF-blocking agents increase or decrease the risk of lymphomas,” said Dr. Furst.
“Any time you alter the immune system, particularly if you're going to suppress the immune system, you might allow the growth of tumors. This has been a theoretical concern for many of our therapies,” explained Dr. Jonas.
According to the majority of current research, the use of disease-modifying anti-rheumatic drugs (DMARDs) doesn't seem to be associated with an increase in cancer risk, said Dr. Solomon.
One difficulty with studying this area is the risk of confounding, noted Dr. Furst. Patients with higher disease activity have a higher risk of lymphoma, and this group is more likely to be given TNF-blocking agents. “Observe carefully,” he said, “but don't get too excited.”
The skin is one area to observe particularly carefully, Dr. Jonas said, citing research that has shown small increases in the risk of skin cancer in patients who took the first biologics to come on the market. Internists should perform regular skin examinations in patients receiving TNF inhibitors and probably all biologic therapies, Dr. Jonas recommended. For patients who've previously had melanoma or pre-melanoma lesions, she plays it safe and stays away from biologic drugs.
The same advice applies for patients with previous hematologic malignancies. “I think that's pretty well accepted, except for the melanoma, but I think the data look strong enough for melanoma that I advise extreme caution,” said Dr. Jonas. But the data do not show that TNF-blocking agents increase the risk of solid tumors, added Dr. Furst.
“I have treated patients [with biologics] who have had solid tumors and were disease-free for many years. When the risk of rheumatoid affecting quality of life and function outweighs the risk of tumors, then you're going to do that. I think this is the time when you have a very frank discussion with your patients about what we know and what we don't know about biologic therapy,” said Dr. Jonas.
Infections
Rheumatologists know more about the connection between the drugs they commonly prescribe and infections. “In particular with the biologic agents, the TNF inhibitors and the other biologic agents that are often used to treat rheumatoid arthritis, there's a significant risk of opportunistic infections—reactivations of tuberculosis, histoplasmosis, coccidioidomycosis,” said Dr. O’Dell.
When patients on these drugs present with signs of infection, the drugs should be stopped and the infection thoroughly investigated. “The FDA came out with some black box warnings on the TNF inhibitors a year and a half ago because people weren't taking lung infections seriously enough in those patients and people were dying of opportunistic infections in the lungs,” Dr. O’Dell said.
To prevent infections, physicians should give appropriate vaccinations, such as pneumococcus, before patients start biologics. If patients are already taking immune-suppressing medications, it's important to be thoughtful, advised Dr. Furst. “They should not use live viral vaccine when these patients are on the drugs. People are using H. zoster; that's a live vaccine—not a good idea,” he said.
Infection prevention can also be a concern when rheumatoid patients are scheduled for surgery. “This is a little controversial. The data is not absolutely clear that these drugs are associated with an increased incidence of perisurgical infections,” said Dr. Furst.
Caution—and many surgeons—would favor stopping immunosuppressive medications before surgery. That course poses some problems, however, said Dr. Jonas. Many of the medications stay in the patient's system for a long time. “The half-lives are really days to weeks. If you're stopping a biologic therapy a week before their surgery, you're essentially not stopping it,” she said.
If you do decide not to stop one of these drugs before surgery, you can at least take advantage of the long half-life and schedule the surgery for right before a dose is due, noted Dr. Furst.
Dr. Jonas favors stopping biologics a month before surgery. But for some patients, the arthritic consequences of halting medications may outweigh the anti-infection benefits. “You really need to balance the risk of infection versus the risk of flare,” she said.
That balance tips in favor of keeping many patients on methotrexate during surgery, Dr. Jonas noted, such as a patient getting a hip or knee replacement.
“The risk of stopping their methotrexate is that their rehab is going to be very difficult,” she said. “If they have severe hand, wrist, shoulder, elbow disease and they're going to be trying to pull themselves up in rehab and therapy, and now they're flaring with the rest of their disease in this period, it can really hamper their recovery.”
Don't continue methotrexate in patients with renal impairment, however, because hospitalized patients can have a decrease in their glomerular filtration rates, leading to drug toxicity.
Another tip: “Patients with long-standing disease, and anybody who's going to have general anesthesia and have an intubation, should have flexion and extension films of the cervical spine,” Dr. Jonas said. If the patients have C1/C2 subluxation, oral intubation could result in spinal cord compromise, so an alternate intubation method should be planned. Anesthesiologists should also be made aware of the risk of cricoarytenoid arthritis, she said.
Other concerns
The new standard of care is DMARDs, and internists have been slower than specialists to get on board. “Virtually 90% to 95% of patients seen in rheumatology practices who have rheumatoid arthritis will be on one of these drugs. When we go to non-rheumatology practices, the rates of use are much lower,” Dr. Solomon said. “If they need help prescribing these drugs, they should call their local friendly rheumatologist.”
The advice may be basic, but it's an easy way for internists to make a difference in the lives of their patients with rheumatoid arthritis.
“It's a lot of routine health care maintenance. Cancer screening, cardiovascular risk factor modification and osteoporosis [treatment] should be part of any good internist's practice but just needs to be practiced with great care for most rheumatoids, because they're at an increased risk for these different adverse events,” concluded Dr. Solomon.