MKSAP Quiz: 2-month history of increased dyspnea
A 48-year-old woman is evaluated for a 2-month history of increased dyspnea, wheezing, and nonproductive cough. She also reports intermittent pain and swelling in the wrists and knees for the past 6 months. She was diagnosed with scleritis of the left eye 1 month ago that improved with glucocorticoid drops. She also had two episodes of right pinna pain, redness, and swelling. Medications are prednisolone acetate ophthalmic and ibuprofen as needed for joint pain.
On physical examination, vital signs are normal. There is no rash. Sclerae are normal. Hearing is normal. The trachea is tender. On lung auscultation, wheezing is heard in both lung fields with no crackles or rubs. Swelling of the wrists and knees is present.
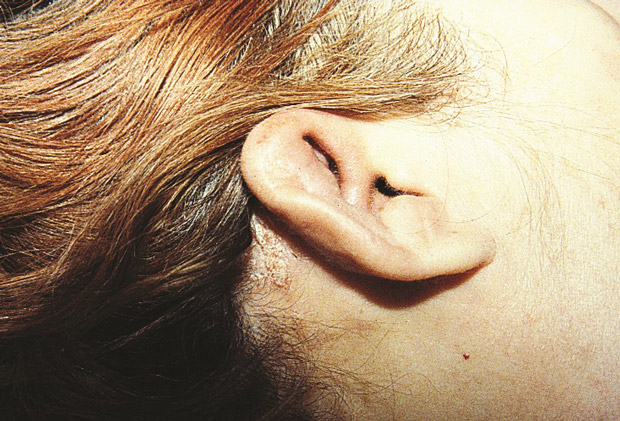
The ear findings are shown.
Laboratory studies show an erythrocyte sedimentation rate of 60 mm/h and a normal complete blood count with differential except for a hemoglobin level of 11 g/dL (110 g/L).
Chest radiograph is normal. CT of the chest reveals bronchial thickening with strictures; there is air trapping distal to the strictures.
Which of the following is the most likely diagnosis?
A. Cogan syndrome
B. Polyarteritis nodosa
C. Relapsing polychondritis
D. Systemic lupus erythematosus
Answer and critique
The correct answer is C. Relapsing polychondritis. This item is Question 49 in the Rheumatology section.
The most likely diagnosis is relapsing polychondritis (RP). RP is characterized by inflammation and damage of cartilaginous tissues; tissues most commonly affected include the cartilaginous portions of the external and middle ear, nose, tracheobronchial tree, and joints. Auricular involvement affects the helix but spares the earlobes. Nasal chondritis can result in collapse of the nasal bridge (saddle nose deformity), which can also be seen in trauma, granulomatosis with polyangiitis, cocaine use, congenital syphilis, and leprosy. Airway stenosis from tracheal ring involvement and aortitis/large-vessel vasculitis may occur and be life-threatening. RP is diagnosed by its typical clinical manifestations. Laboratory tests are nonspecific; acute phase reactants are elevated in 80%, and mild anemia is present in 44%. Patients with RP should undergo imaging (CT or MRI) to evaluate the large airways for inflammation/stenosis. This patient has a history of recurrent inflammation of the cartilage of the right ear, inflammatory eye disease, inflammatory arthritis, and bronchial strictures due to inflammation of bronchial cartilage, consistent with a diagnosis of RP.
Cogan syndrome (interstitial keratitis, with cochlear and vestibular dysfunction) is an unlikely diagnosis because the patient has neither vestibular nor cochlear findings.
Polyarteritis nodosa, a medium-vessel vasculitis, affects the mesenteric and renal arteries. Patients usually present with abdominal symptoms, neurologic involvement, and skin findings. Polyarteritis nodosa does not involve the eye or cartilage of the ear, nose, or airways, making this an unlikely diagnosis.
Besides the inflammatory arthritis, this patient has no typical symptoms or signs of systemic lupus erythematosus (SLE). In addition, SLE does not typically cause inflammation and destruction of cartilaginous structures.
Key Point
- Relapsing polychondritis is characterized by inflammation and damage of cartilaginous tissues; tissues most commonly affected include the cartilaginous portions of the external and middle ear, nose, tracheobronchial tree, and joints.



