MKSAP Quiz: 1-month history of a skin ulcer
A 24-year-old woman is evaluated for a 1-month history of increasing pain and bleeding from a skin ulcer next to her stoma. The skin symptoms get worse each time she changes her appliance. She underwent proctocolectomy 4 years ago for medically refractory colonic Crohn disease. She has not had small-bowel involvement, and her ostomy output has been stable since surgery.
On physical examination, vital signs are normal. The skin findings are shown.
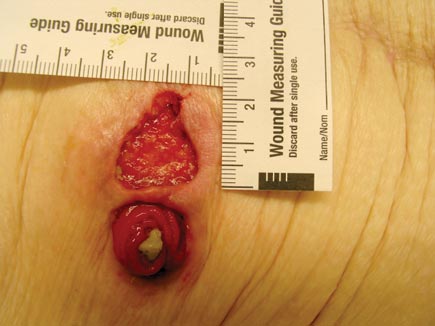
The remainder of the skin examination is normal. The abdomen is soft with normal bowel sounds. There is no distention, tenderness, masses, or organomegaly.
Which of the following is the most likely cause of this patient's skin findings?
A. Acrodermatitis enteropathica
B. Erythema nodosum
C. Pyoderma gangrenosum
D. Squamous cell carcinoma
Answer and critique
The correct answer is C: Pyoderma gangrenosum. This question can be found in MKSAP 17 in the Gastroenterology and Hepatology section, item 26.
This patient's ulcerating lesion is characteristic of pyoderma gangrenosum (PG). PG is an uncommon skin disease characterized by intense neutrophilic inflammation and invasion of the skin. Lesions are classically ulcerated, but PG may also present with bullae, pustulonodules, and vegetative plaques. Typical lesions begin as painful pustules that rapidly ulcerate and expand, with an edematous, rolled, or undermined-appearing border that may have a violaceous hue. Annular rings are sometimes noted. As with other neutrophilic dermatoses, when the process is active, approximately 25% of patients will exhibit pathergy or induction of new lesions at sites of trauma, including ostomy, phlebotomy, and intravenous sites. Peristomal PG, occurring around ostomy sites, is common and can be challenging to manage. As PG resolves, it tends to heal with atrophic scarring in a cross-like or cribriform pattern. There are no definitive diagnostic tests, and PG is a diagnosis of exclusion. Skin biopsy may be required to exclude other diseases such as cutaneous Crohn disease but may cause worsening of the PG. Treatment can be challenging, and if there is an associated underlying disease, therapy should be directed at controlling that process. Extraintestinal manifestations such as oral aphthous ulcers, arthralgia, inflammatory eye diseases, and PG are seen in approximately 10% of patients with inflammatory bowel disease.
Acrodermatitis enteropathica (AE) is an inherited or acquired metabolic disorder characterized by perioral and acral (in the extremities) erythematous and vesiculobullous dermatitis and alopecia related to zinc deficiency. AE has been associated with Crohn disease, but this patient's stomal ulcer is not consistent with AE.
Erythema nodosum is the most common cutaneous manifestation of inflammatory bowel disease, occurring in up to 20% of patients, particularly women. The lesions of EN are tender, subcutaneous nodules presenting as barely appreciable convexities on the skin surface, with a reddish hue in the acute phase. EN is frequently bilateral and symmetrical, and it usually occurs on the distal lower extremities, but it may also appear on the trunk, thighs, or upper extremities.
Squamous cell carcinoma (SCC) usually appears as a scaly, crusted, well-demarcated red papule, plaque, or nodule. SCC can develop in patients with Crohn disease, most commonly at sites of chronic, long-standing inflammation such as chronic fistulas. This patient's ulcerative skin lesion with undermined and violaceous borders is not consistent with the appearance of SCC.
Key Point
- Pyoderma gangrenosum (PG) is characterized by painful pustules that rapidly ulcerate and expand, with edematous, rolled, or undermined borders that may have a violaceous hue; PG may be an extraintestinal manifestation of Crohn disease.



