MKSAP Quiz: Ulcerating, painful lesion
A 72-year-old man is evaluated for an ulcerating, painful lesion on his left calf that began as a patch of red skin 2 to 3 weeks ago. He has dialysis-dependent end-stage kidney disease, atrial fibrillation, and hypertension.
Medications are amlodipine, calcium acetate, calcitriol, insulin, and warfarin. There have been no recent changes in his medications.
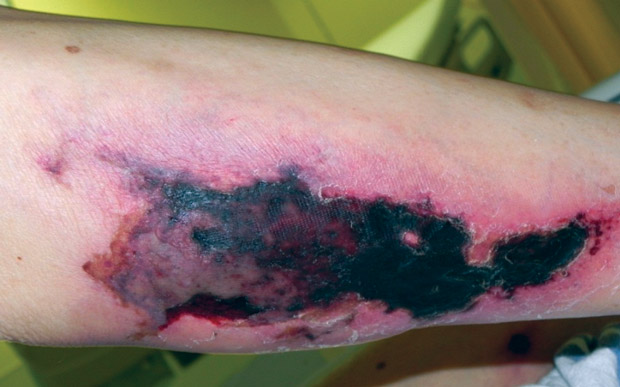
On physical examination, vital signs are normal. Skin findings are shown. There are no other skin changes, lesions, or rash.
Laboratory studies:
| INR | 2.5 |
| Calcium | 9.6 mg/dL (2.4 mmol/L) |
| Phosphorus | 3.1 mg/dL (1.0 mmol/L) |
| Parathyroid hormone | 361 pg/mL (361 ng/L) |
A skin punch biopsy shows calcifications in the subcutaneous tissue within necrotic lipocytes and within the walls of small blood vessels. There is confluent epidermal necrosis.
Which of the following is the most likely diagnosis?
A. Calciphylaxis
B. Leukocytoclastic vasculitis
C. Venous stasis ulcer
D. Warfarin skin necrosis
Answer and critique
The correct answer is A. Calciphylaxis. This item is Question 47 in MKSAP 19's Nephrology section.
The most likely diagnosis is calciphylaxis (calcific uremic arteriolopathy) (Option A). This patient with dialysis-dependent end-stage kidney disease (ESKD) has developed a painful ulcer on the left calf with central necrosis and a skin biopsy showing vascular calcification. Calciphylaxis develops from pathologic calcifications in the dermal arterioles, leading to thrombosis, ischemia, and necrosis of the overlying skin. It is a painful and often life-threatening complication of ESKD and is associated with a high risk of mortality due to secondary infection and sepsis. Many patients with calciphylaxis have severe secondary hyperparathyroidism and elevated calcium-phosphorous product. However, patients such as this one with normalized serum calcium and phosphate levels are also at risk; calciphylaxis is an increasingly recognized complication of ESKD in the dialysis community. There are no FDA-approved treatments for calciphylaxis. However, calcimimetics are used to suppress parathyroid hormone, and data from a large study show fewer cases of calciphylaxis among treated patients. Sodium thiosulfate, an anti-inflammatory agent, is also routinely used for patients with calciphylaxis.
Leukocytoclastic vasculitis (Option B) should be considered in the differential diagnosis of a nonhealing leg ulcer, but patients typically present with palpable purpura, not a rapidly advancing cutaneous ulcer, and the biopsy would show perivenular and intramural inflammatory infiltrates rather than the vascular calcifications seen in this patient.
Venous stasis ulcers (Option C), a chronic skin condition associated with other signs of venous insufficiency (edema, varicosities, hyperpigmentation), are irregularly shaped, shallow, and often weep serous fluid. The ulcers are rarely necrotic. The sudden appearance of a necrotic ulcer is not indicative of a venous ulcer.
Although warfarin-related necrosis could cause necrotic skin ulceration (Option D), it would be expected to occur when the agent was initiated, often with large loading doses, and would not show calcifications in the underlying vessel walls on biopsy but rather thrombosis.
Key Points
- Calciphylaxis (calcific uremic arteriolopathy) is characterized by calcifications in the dermal arterioles resulting in painful ischemic skin lesions and is an increasingly recognized complication of end-stage kidney disease.
- Many patients with calciphylaxis have severe secondary hyperparathyroidism and elevated calcium-phosphorous product.



