MKSAP Quiz: 4-month history of cough, chest pressure
A 49-year-old man is evaluated for a 4-month history of cough, chest pressure, and double vision. He has no fever, night sweats, or weight loss. He has never smoked.
On physical examination, vital signs are normal. There is ptosis bilaterally. The remainder of the physical examination is normal.
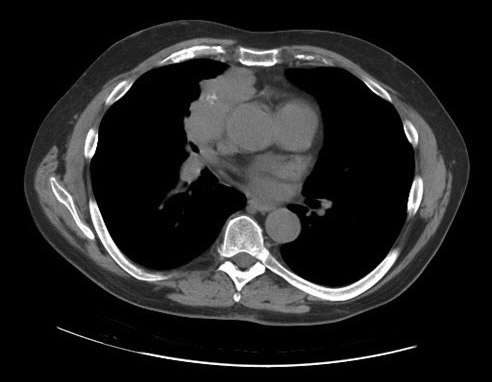
A CT scan of the chest is shown.
Which of the following is the most appropriate test to perform next?
A. Acetylcholine receptor antibody
B. a-Fetoprotein
C. b-Human chorionic gonadotropin
D. Lactate dehydrogenase
Answer and critique
The correct answer is A. Acetylcholine receptor antibody. This item is Question 48 in MKSAP 18's Pulmonary and Critical Care Medicine section.
An acetylcholine receptor (AChR) antibody test should be ordered. The mediastinum can be divided into three separate compartments (anterior, middle, and posterior), which can help narrow the differential diagnosis of a mediastinal mass. Each compartment normally contains separate and distinct anatomic structures that can lead to development of a mass. Patients may be asymptomatic and are often diagnosed after obtaining a chest radiograph for another reason, whereas others present with symptoms related to compression of adjacent structures. For example, they may present with dyspnea if the airway is compressed from a nearby mass or with upper extremity edema if vascular structures are compressed.
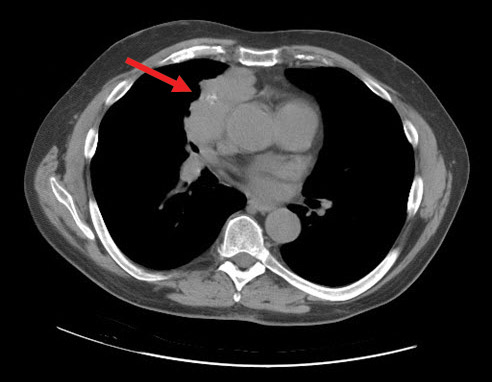
This patient has an anterior mediastinal mass (arrow) and neurologic symptoms. Masses in this location are usually remembered as the “terrible T's”: thymoma, teratoma/germ cell tumor, “terrible” lymphoma, and thyroid. Additional considerations include thoracic aneurysm. Thymomas are the most common cause of an anterior mediastinal mass. Patients usually present as middle-age adults and may develop paraneoplastic syndromes. For example, myasthenia gravis can develop in 30% to 50% of patients with a thymoma. In comparison, only 10% to 15% of patients with myasthenia gravis have a thymoma. The second most common cause is lymphoma; these patients are typically younger at the time of presentation. Other less common paraneoplastic syndromes include pure red blood cell aplasia, nonthymic cancers, and acquired hypogammaglobulinemia.
Myasthenia gravis is an autoimmune disorder of the neuromuscular junction that is characterized by fatigable (or fluctuating) muscular weakness. Common symptoms are ptosis and diplopia, which this patient has. Diagnosis of myasthenia gravis is based on clinical findings, detection of disease-specific antibodies (acetylcholine receptor antibodies in 90% of patients and anti–muscle-specific kinase [MuSK] antibodies in another 5% [with 5% of patients remaining antibody negative]), and electromyography findings (such as a characteristic decremental response to repetitive stimulation). Thymectomy should be performed in all patients with thymoma.
a-Fetoprotein and b-human chorionic gonadotropin are commonly elevated in germ cell tumors, which are also part of the differential diagnosis of an anterior mediastinal mass. However, this patient also has symptoms of myasthenia gravis, which is not associated with germ cell tumors.
Lactate dehydrogenase is commonly elevated in lymphoma and seminomas but is not as specific as other tumor markers and will not help determine the cause of this patient's symptoms.
Key Point
- Masses in the anterior mediastinum are usually recalled as the “terrible T's”: thymoma, teratoma/germ cell tumor, “terrible” lymphoma, and thyroid.




