MKSAP Quiz: 3-month history of rash
A 46-year-old woman is evaluated for a 3-month history of a rash during the summertime. She is otherwise well and takes no medications.
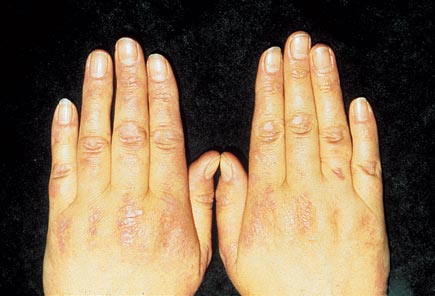
On physical examination, vital signs are normal. BMI is 23. Examination of the skin reveals eyelid swelling and a periorbital violaceous rash, erythema and poikiloderma of the anterior chest and upper back, and an erythematous papular rash on the hands; there is no malar eruption, skin thickening, or digital ulcers. Muscle strength and reflexes are normal.
The appearance of the hands is shown.
Electromyogram and chest radiograph are normal.
Laboratory studies:
| Complete blood count | Normal |
| Chemistry panel | Normal |
| Aldolase | 5.1 U/L (normal range, 1.0-8.0 U/L) |
| Creatine kinase | 100 U/L |
| Antinuclear antibodies | Titer of 1:640 |
| Anti–Jo-1 antibodies | Negative |
| Urinalysis | Normal |
Which of the following is the most likely diagnosis?
A. Amyopathic dermatomyositis
B. Polymorphous light eruption
C. Rosacea
D. Systemic lupus erythematosus
Answer and critique
The correct answer is A: Amyopathic dermatomyositis. This question can be found in MKSAP 17 in the Rheumatology section, item 4.
The most likely diagnosis is amyopathic dermatomyositis. This patient has a clinical presentation of heliotrope eruption in the form of a violaceous periorbital rash, Gottron papules over the extensor surface of small joints of the hands, and photodistributed violaceous poikiloderma (V sign and Shawl sign) without muscle weakness. These are findings of skin involvement seen in dermatomyositis without any clinical, serum, or electromyogram (EMG) findings of muscle involvement or myositis, suggesting the diagnosis of amyopathic dermatomyositis. Amyopathic dermatomyositis is seen in about 20% to 25% of patients with dermatomyositis, but some of these patients have evidence of myositis on one of the evaluation studies (muscle enzymes, EMG, or muscle biopsy) in the absence of muscle weakness. To qualify for the diagnosis of amyopathic dermatomyositis, the patient should have the characteristic rash but no clinical, laboratory, or muscle evaluation findings of myositis. Amyopathic dermatomyositis may be triggered by sunlight exposure and also is associated with an underlying malignancy. Treatment is usually with glucocorticoids and immunosuppressive agents.
Polymorphous light eruption (PMLE) is another dermatologic condition in which patients develop skin lesions after exposure to sunlight; these lesions last several days and resolve spontaneously in the absence of reexposure. A variety of skin lesions may be seen in PMLE, including urticarial wheals, papules, plaques, and vesicles. PMLE usually develops early in the spring, with the first few exposures to sunlight, and can be triggered by intense exposures. These lesions occur in photodistributed areas but lack characteristic heliotrope or Gottron eruptions. A diagnosis of PMLE is unlikely in this patient.
Rosacea is a chronic, inflammatory condition that causes an acneiform eruption and flushing on the mid-face. There are two types, vascular and papular pustular (inflammatory) rosacea. Vascular rosacea presents as persistent flushing, especially of the central face, with prominent telangiectasias. Pustules and papules are seen in the inflammatory variant, but in contrast to acne, rosacea pustules are not follicular based. The patient's findings are not consistent with rosacea.
Although this patient has positive antinuclear antibodies, she lacks the associated findings of systemic lupus erythematosus (SLE), including malar/discoid rash, arthritis, organ involvement, and kidney disease. SLE can cause a rash on the hands similar to Gottron papules, but it more typically involves skin located between the joints.
Key Point
- Amyopathic dermatomyositis refers to dermatomyositis with cutaneous involvement in the absence of clinical, laboratory, electromyogram, or biopsy evidence of myositis.