MKSAP Quiz: 3-month history of hand pain
A 46-year-old woman is evaluated for a 3-month history of pain and swelling of the hands, dyspnea, and wheezing. She has no other pertinent personal or family medical history. She takes naproxen as needed for pain relief.
On physical examination, vital signs are normal. The ears are thickened bilaterally; the right ear has moderate warmth, erythema, and tenderness to palpation. Saddle nose deformity is noted; examination of the nares shows intact mucosa. Tenderness of the metacarpophalangeal and proximal interphalangeal joints is noted; the second and third metacarpophalangeal joints are swollen bilaterally. Pulmonary examination reveals expiratory wheezing in the upper lung fields. The appearance of the ears is shown.
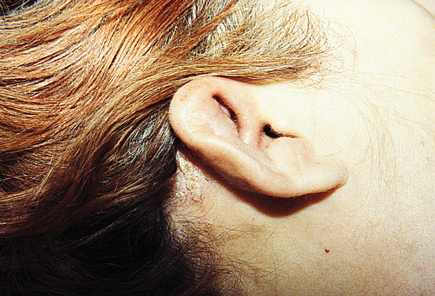
Laboratory studies reveal a hemoglobin level of 11 g/dL (110 g/L) and an erythrocyte sedimentation rate of 56 mm/h. Antinuclear antibody and ANCA assay results are negative.
Chest radiograph is normal.
Which of the following is the most appropriate diagnostic test to perform next in this patient?
A. CT of the sinuses
B. Pulmonary function testing with flow volume loops
C. Rheumatoid factor
D. Urine toxicology screen
Answer and critique
The correct answer is B) Pulmonary function testing with flow volume loops. This question can be found in MKSAP 16 in the Rheumatology section, item 45.
Pulmonary function testing with flow volume loops is indicated for this patient with suspected relapsing polychondritis and pulmonary findings. This autoimmune inflammatory disorder affects the cartilage of the ears and nose, and up to 50% of patients also have a rheumatoid arthritis like polyarthritis. Relapsing polychondritis also can affect the cartilaginous tracheal rings of the larynx, trachea, and bronchi, which can lead to obstructive findings on flow volume loop diagrams. There are no serologic tests for relapsing polychondritis; diagnosis can be made by biopsy of the affected cartilage but is not necessary if sufficient clinical criteria are present, as seen in this patient with chondritis of the ears and nose, along with a polyarthritis. Because respiratory tract involvement is prevalent, pulmonary function testing with flow volume loops is indicated for patients diagnosed with or suspected of having relapsing polychondritis. This testing can detect the presence of large upper airway involvement, which might require more aggressive treatment.
Saddle nose deformity also can occur in patients with granulomatosis with polyangiitis (also known as Wegener granulomatosis) and is caused by destructive sinusitis with erosion into the cartilage, which can be detected by performing a CT of the sinuses. This patient's previous ear inflammation, negative ANCA, and absence of sinus disease argue against granulomatosis with polyangiitis as the cause of saddle nose deformity, and CT is not warranted.
Rheumatoid factor is present in many patients with rheumatoid arthritis, a disorder that is not associated with destructive facial lesions.
Patients with nasal deformity suspected to be caused by cocaine-induced midline destructive disease or vasculitis would require a urine toxicology screen. These patients often have a positive (“atypical”) pANCA due to antibodies to elastase (rather than myeloperoxidase). Based on this patient's findings, including ear damage, arthritis, and negative ANCA, a urine toxicology screen is not warranted.
Key Point
- Pulmonary function testing with flow volume loops is indicated for patients diagnosed with or suspected of having relapsing polychondritis to evaluate for large upper airway involvement.