MKSAP Quiz: 6-week history of dyspnea, cough
A 64-year-old woman is evaluated for a 6-week history of dyspnea, dry cough, fever, chills, night sweats, and fatigue, which have not responded to treatment with azithromycin and levofloxacin; she has lost 2.2 kg (5 lb) during that time. The patient had a thorough examination 6 months ago while she was asymptomatic that included routine laboratory studies, age- and sex-appropriate cancer screening, and a chest radiograph; all results were normal. The patient has never smoked, has had no known environmental exposures, and has not traveled recently or been exposed to anyone with a similar illness. Her only medications are aspirin and a multivitamin.
On physical examination, temperature is 37.8°C (100.0°F); other vital signs are normal. Cardiac examination is normal. There are scattered crackles in the mid-lung zones with associated rare expiratory wheezes. There is no digital clubbing. Musculoskeletal and skin examinations are normal. Chest radiograph is shown.
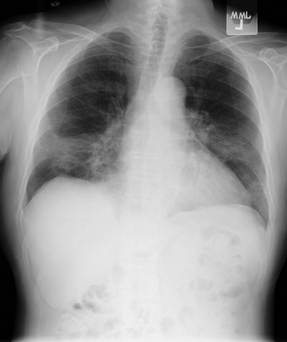
Which of the following is the most likely diagnosis?
A. Cryptogenic organizing pneumonia
B. Idiopathic pulmonary fibrosis
C. Lymphocytic interstitial pneumonia
D. Nonspecific interstitial pneumonia
Answer and Critique
The correct answer is A: Cryptogenic organizing pneumonia. This question can be found in MKSAP 15 in the Pulmonology and Critical Care Medicine section, item 20.
This nonsmoker without any exposure history has acute to subacute development of nonspecific systemic and respiratory symptoms with a dominant alveolar (opacification) process on chest radiograph. The tempo of the disease process is the key to differentiating cryptogenic organizing pneumonia (COP) from other interstitial lung diseases. COP (formerly called idiopathic bronchiolitis obliterans organizing pneumonia) is often acute or subacute, with symptom onset occurring within 2 months of presentation in three fourths of patients. The presentation is so suggestive of an acute or subacute lower respiratory tract infection that patients have almost always been treated with and failed to respond to one or more courses of antibiotics before diagnosis.
Idiopathic pulmonary fibrosis (IPF), nonspecific interstitial pneumonia (NSIP) or lymphocytic interstitial pneumonia (LIP) typically follows a prolonged course with evidence of respiratory symptoms and radiographic findings that progress slowly over months or years. Radiographic findings in COP are also distinct from those in IPF, NSIP and LIP. A dominant alveolar opacification process is typically present in patients with COP. The opacities are almost always bilateral with varied distribution. One of the key radiographic features of COP is the tendency for COP opacities to “migrate” or involve different areas of the lung on serial examinations. Although the radiographic findings of IPF, NSIP and LIP are varied, they all have a dominant interstitial (reticular) pattern with or without opacities. LIP (which is very rare) is one of the few interstitial lung diseases that can present with cystic changes on high-resolution CT.
Key Point
- Cryptogenic organizing pneumonia most often presents with subacute disease progression and bilateral opacities on chest radiograph.


