MKSAP Quiz: Red, scaly skin lesions
A 37-year-old man is evaluated for a 4-month history of progressively worsening red, scaly lesions involving the scalp, trunk, and extremities. During the past month, he also has had pain in the hands and feet and has lost 4.5 kg (10.0 lb). Aspirin and acetaminophen have helped to relieve his joint symptoms. He does not drink alcoholic beverages, has no other medical problems, and takes no additional medications. He denies allergies. He has sex with men and women and uses condoms inconsistently.
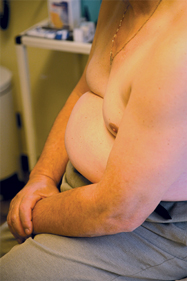
On physical examination, vital signs are normal. The appearance of lesions found on the arms, hands, upper torso, back, inside the umbilicus, and legs is shown.
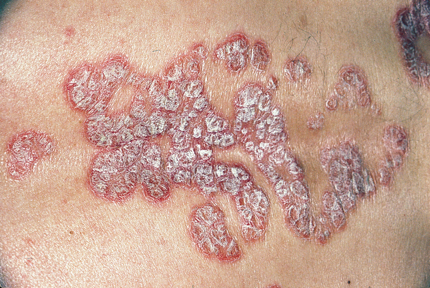
There is swelling of the first and fourth digits on the left hand and of the feet. The left first metatarsophalangeal joint and left ankle are swollen and tender to palpation.
Which of the following diagnostic studies should be performed next in this patient?
A. Anti-cyclic citrullinated peptide antibody assay
B. Antinuclear antibody assay
C. Hepatitis C virus antibody assay
D. HLA-B27 testing
E. Serologic testing for HIV antibodies
Answer and Critique
The correct answer is E: Serologic testing for HIV antibodies. This question can be found in MKSAP 15 in the Rheumatology section, item 4.
This patient should be tested for HIV infection. He has extensive new-onset psoriasis accompanied by asymmetric peripheral arthritis that predominantly involves the small joints and dactylitis. This constellation of symptoms is consistent with psoriatic arthritis. Psoriasis, psoriatic arthritis, or reactive arthritis may be presenting signs of HIV infection or may appear after the diagnosis of HIV infection is established. Compared with psoriasis that develops in the general population, HIV-associated psoriasis is more likely to have an explosive onset and more severe disease course that may include nail changes, palmar and plantar involvement, and erythroderma. Underlying HIV infection should therefore be excluded in all patients with new-onset psoriasis or psoriatic arthritis, as well as in those with mild forms of these conditions who experience an explosion of their disease. Diagnosis of HIV infection is important for the purposes of identifying and managing a comorbidity but also because a patient's immune status may affect the selection of treatment for psoriasis; for example, immunosuppressive therapy would not be indicated in a patient with HIV infection.
The presence of anti-cyclic citrullinated peptide antibodies is relatively specific for rheumatoid arthritis. However, rheumatoid arthritis is unlikely in a patient with an asymmetric pattern of joint disease and would not explain the temporal association between this patient's arthritis and new-onset psoriasis.
Patients with systemic lupus erythematosus (SLE) and hepatitis C virus infection may have musculoskeletal and cutaneous manifestations. However, joint involvement in SLE, which is associated with antinuclear antibodies, typically manifests as symmetric arthritis that involves the small and large joints. In addition, patients with SLE may present with many types of cutaneous lesions, including photosensitivity, malar rash, subacute cutaneous lupus, and discoid lupus. However, none of these conditions resembles the erythematous plaque with a thick silvery scale that is characteristic of chronic plaque psoriasis.
Joint involvement in patients with hepatitis C virus infection also is more likely to be symmetric and more commonly manifests as arthralgia instead of frank arthritis. Furthermore, skin disease in these patients usually consists of ulcerations and purpuric rash that is often limited to the lower extremities.
The spondyloarthropathies are associated with an increased incidence of HLA-B27 compared with the general population. However, patients with psoriatic arthritis that predominantly manifests as peripheral joint involvement are only slightly more likely to have HLA-B27 than the general population. Furthermore, most HLA-B27-positive patients do not develop a spondyloarthropathy. This study therefore would not help to diagnose this patient's condition because it lacks both sensitivity and specificity.
Key Point
- Underlying HIV infection should be excluded in all patients with new-onset psoriasis or psoriatic arthritis, as well as in those with mild forms of these conditions who experience an explosion of their disease.