MKSAP Quiz: Persistent itching, odor of the feet
A 19-year-old man is evaluated for 4 to 5 months of persistent itching, thickening of the skin, and odor of the feet. He also has hyperhidrosis of the palms and soles. Medical history is otherwise unremarkable, and he takes no medications.
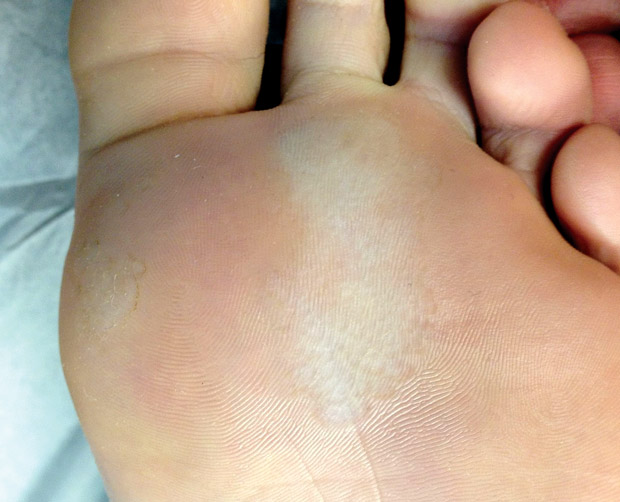
On physical examination, vital signs are normal. Skin findings are shown.
There is substantial odor of the feet. There are no changes to the toenails. The axillae and groin are unremarkable.
Potassium hydroxide preparation of skin scrapings does not reveal fungal elements.
Which of the following is the most likely diagnosis?
A. Aquagenic keratoderma
B. Erythrasma
C. Keratoderma blenorrhagicum
D. Pitted keratolysis
E. Tinea pedis
Answer and critique
The correct answer is D. Pitted keratolysis. This item is Question 44 in MKSAP 18's Dermatology section.
Pitted keratolysis is a bacterial infection most commonly caused by Kytococcus sedentarius. The key features are waxy or scaly plaques, thickening of the plantar skin (keratoderma), small punctate erosions in the plaques that may coalesce to form broader erosions, and odor. Risk factors for infection include excess sweating (hyperhidrosis) and prolonged occlusion of the feet in footwear. Usually symptoms are minimal, with most complaints directed toward odor, but minor itching can occur. Treatment is best accomplished with topical antibiotics and keeping the feet dry, including the use of topical antiperspirants.
Aquagenic keratoderma presents with wrinkling, translucency, and scaling of the palmar hands and plantar feet shortly after exposure to water and is associated with carrier status of the cystic fibrosis gene. Aquagenic keratoderma does not feature pitting.
Erythrasma is also a bacterial infection that tends to involve intertriginous areas such as the axillae and the crural folds. Skin may develop a finely wrinkled, cigarette paper texture, but would not feature pitting. Erythrasma will fluoresce to a coral red color with a Wood lamp examination because of bacterial porphyrin production.
Keratoderma blenorrhagicum is a keratoderma of the palms or soles associated with reactive arthritis. With this rash, patients develop psoriasiform red plaques with lamellar scale. Patients may have other features of reactive arthritis such as asymmetric monoarthritis or oligoarthritis in the lower extremities, enthesopathy, dactylitis, and sacroiliitis.
Tinea pedis can cause scaling and itching of the feet. Patients typically develop pink or red scaly plaques with a serpiginous or arcuate discrete border. Scale is often emphasized at the edge of plaques. Pustules may be present at hair follicles, but pitting and strong odor are not typical. Potassium hydroxide preparation of skin scrapings should reveal fungal elements, except in partially treated cases.
Key Point
- Pitted keratolysis is a superficial bacterial infection characterized by small pits and punctate erosions primarily on the plantar aspects of the feet; risk factors include increased perspiration (hyperhidrosis) and prolonged occlusion of the feet.