MKSAP Quiz: Decreased exercise tolerance
A 62-year-old woman is evaluated for a 4-month history of decreased exercise tolerance, joint stiffness, mild weakness, and a rash on her hands. She has noted increasing difficulty carrying heavy objects and feels exhausted after climbing stairs. Although her joints are stiff, she has not had any joint swelling. Her rash developed around the time of her other symptoms and has not responded to over-the-counter topical agents. She has no other symptoms, including cough or dyspnea. Medical history is unremarkable, and she takes no medications.
On physical examination, temperature is 37.2°C (99.0°F), blood pressure is 109/72, pulse rate is 82/min, and respiration rate is 20/min. Oxygen saturation is 98% on ambient air. Cardiopulmonary examination is unremarkable. Joint examination is normal. Skin findings are shown.
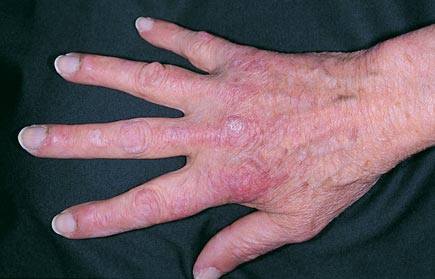
A plain chest radiograph is normal.
Laboratory studies:
| Creatine kinase | 320 U/L |
| Antinuclear antibodies | Positive (titer of 1:640) |
| Anti-dsDNA antibodies | Negative |
| Anti-Ro/SSA antibodies | Negative |
| Anti-La/SSB antibody | Negative |
| Complete blood count | Normal |
| Metabolic profile | Normal |
Which of the following pulmonary conditions is associated with this patient's clinical presentation?
A. Bronchiectasis
B. Diffuse alveolar hemorrhage
C. Hilar lymphadenopathy
D. Interstitial lung disease
E. Pleuritis
Answer and critique
The correct answer is D: Interstitial lung disease. This question can be found in MKSAP 17 in the Dermatology section, item 18.
This patient has a clinical picture consistent with dermatomyositis, and she is at increased risk for developing interstitial lung disease. Polymyositis and dermatomyositis are idiopathic inflammatory myopathies. Dermatomyositis also has various characteristic cutaneous manifestations. There are two forms of dermatomyositis: the classic form with both skin and muscle inflammation and either hypomyopathic or amyopathic dermatomyositis with skin findings but minimal or absent muscle inflammation. Patients with polymyositis and those with any form of dermatomyositis (classic, hypomyopathic, or amyopathic) are at increased risk for malignancy, with patients with dermatomyositis at higher risk than those with polymyositis. Similarly, patients with polymyositis or dermatomyositis (regardless of subtype) are at risk for developing interstitial lung disease. Several histopathologic patterns of interstitial lung disease are associated with polymyositis and dermatomyositis. Patients with certain serologic abnormalities may be at higher risks for interstitial lung disease, such as those with anti-Jo-1 antibody positivity. Current screening recommendations include performing pulmonary function tests with measurement of DLCO. Patients often require additional testing, including high-resolution chest CT scans. In patients with mild disease, observation may be appropriate. Increasing levels of immunosuppression may be required for patients with more severe interstitial lung disease.
Bronchiectasis is an acquired disorder characterized by permanent abnormal dilatation and destruction of the bronchial walls and requires an infectious insult plus impaired bronchial drainage to develop. Bronchiectasis is an uncommon finding in patients with dermatomyositis, and this patient has no clinical findings consistent with this diagnosis, including existing pulmonary disease, cough, or sputum production.
Diffuse alveolar hemorrhage may occur in a variety of settings, including in patients with active pulmonary vasculitis. Diffuse alveolar hemorrhage is a rare complication in patients with dermatomyositis and is inconsistent with this patient's clinical features.
Hilar lymphadenopathy is often seen in patients with sarcoidosis; the skin manifestations of sarcoidosis, if present, include violaceous infiltrated papules around the nasal ala and periorbitally or periorally or within scars or tattoos. This patient's skin findings are not consistent with a diagnosis of sarcoidosis.
Pleuritis is an uncommon pulmonary complication of systemic lupus erythematosus (SLE). Generally this will occur in patients with true SLE, as opposed to the cutaneous forms of lupus such as chronic cutaneous lupus erythematosus (discoid lupus). Patients with SLE will generally have a bright red patch symmetrically over their cheeks, the so-called butterfly or malar rash.
Key Point
- Dermatomyositis is associated with an increased risk of interstitial lung disease.