MKSAP Quiz: 1-week history of discharge
A 25-year-old woman is evaluated for a 1-week history of malodorous vaginal discharge associated with vulvar itching and burning. She is sexually active and has had three partners in the past 6 months. She has no history of sexually transmitted infection.
On physical examination, vital signs are normal. BMI is 22. There is a thin, gray, homogeneous discharge coating the vaginal walls. There are no external genital lesions and no vulvar erythema or excoriations. The cervix appears normal. There is no cervical motion tenderness or adnexal tenderness. Vaginal pH is 6.0, “whiff” test is positive. Results of saline microscopy are shown. Microscopy after the addition of potassium hydroxide does not show hyphae or pseudohyphae. A urine pregnancy test is negative.
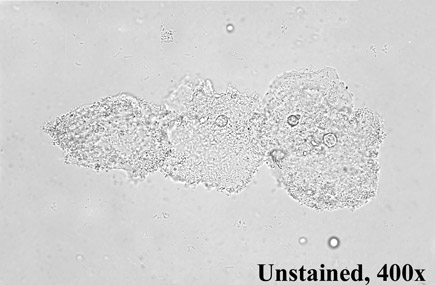
Which of the following is the most appropriate treatment?
A. Clotrimazole cream, 7-day topical regimen
B. Fluconazole, single-dose oral regimen
C. Metronidazole, 7-day oral regimen
D. Metronidazole, single-dose oral regimen
Answer and Critique
The correct answer is C: Metronidazole, 7-day oral regimen. This question can be found in MKSAP 16 in the General Internal Medicine section, item 111.
The most appropriate treatment for this patient is a 7-day oral regimen of metronidazole (500 mg twice daily). She has bacterial vaginosis (BV), a polymicrobial infection characterized by an overgrowth of multiple anaerobic bacteria. Although BV is not a sexually transmitted infection, risk factors include lack of condom use and multiple or new sexual partners. BV can be diagnosed clinically using Amsel criteria, which include the following symptoms or signs: (1) homogeneous thin discharge that coats the vaginal walls; (2) clue cells (epithelial cells with borders obscured by small bacteria) on saline microscopy; (3) pH of vaginal fluid >4.5; and (4) fishy odor of vaginal discharge before or after the addition of 10% potassium hydroxide to the secretions (the “whiff” test). The presence of at least three of these clinical findings has a high sensitivity and specificity for diagnosing BV when compared with Gram stain of collected secretions, which is the gold standard. Because this woman is symptomatic, treatment should be offered with either oral metronidazole, vaginal metronidazole gel, or vaginal clindamycin cream; patient preference should dictate treatment choice. Topical clindamycin should be avoided during pregnancy as it may increase the risk of adverse outcomes. Women treated with oral metronidazole should be cautioned to avoid alcohol, which can cause a disulfiram-like reaction.
This patient's abnormal vaginal pH and lack of yeast and hyphae on potassium hydroxide preparation make vulvovaginal candidiasis an unlikely explanation for her symptoms. Treatment with oral fluconazole or topical clotrimazole cream, effective therapies for vulvovaginal candidiasis, is not warranted.
This patient has multiple sexual partners, increasing her risk for trichomoniasis. Characteristic symptoms and signs include a malodorous discharge with vulvar itching, burning, and postcoital bleeding. Although the vaginal pH will be elevated and the whiff test may be positive (as noted with this patient), clue cells are not a characteristic finding on saline microscopy, making trichomoniasis an unlikely diagnosis in this patient.
Oral metronidazole is also used for the treatment of trichomoniasis, but it is typically given as a single 2-g dose, which would not be appropriate for treatment of BV.
Key Point
- Bacterial vaginosis is the likely diagnosis in women with at least three of the following features: (1) homogeneous thin discharge that coats the vaginal walls; (2) clue cells on saline microscopy; (3) pH of vaginal fluid >4.5; and (4) fishy odor of vaginal discharge (positive “whiff” test).




